- Topics
- What is Prader-Willi Syndrome?
- What are the Symptoms of Prader-Willi Syndrome?
- Infants
- Early Childhood to Adulthood
- How is Prader-Willi Syndrome diagnosed?
- How does Prader-Willi Syndrome affect developmental milestones?
- Prader-Willi Syndrome and Behavioural Issues
- Prader-Willi Syndrome and Eating Habits
- When to See a Doctor About Prader-Willi Syndrome
- How Common is Prader-Willi Syndrome?
- What Causes Prader-Willi Syndrome?
- Summary:
- How Prader-Willi Syndrome Impacts the Hypothalamus
- Complications of Prader-Willi Syndrome
- Obesity-related complications
- Insufficient hormone production complications
- Other complications
- What Are the Symptoms of Prader-Willi Syndrome?
- Summary:
- Increased appetite and high propensity to obesity
- Low muscle mass and muscle tone
- Behavioural and mental health issues
- Other symptoms of Prader-Willi Syndrome
- Navigating Prader-Willi Syndrome – Support is Available for You and Your Loved Ones
- What Treatments are Available for Prader-Willi Syndrome?
- Common symptoms associated with PWS
- Treatment options for people with PWS
- Weight management
- Mental health and behavioural treatments
- Sleep treatments
- Growth and sex hormone therapy
- Care and attention to individual needs
- The Future for People with Prader-Willi Syndrome
- Accessing Supports for Prader-Willi Syndrome in Sydney
- Support for Infants and Children with Prader-Willi Syndrome
- Seek Valuable Specialist Care Where Possible
- Genetic Counselling and Prader-Willi Syndrome
- Support for Adults with Prader-Willi Syndrome
- Maintain medical care and Intervention therapies
- Regular and supported employment
- Recreation and Community Engagement
- Accommodation and Housing
- Other Lifestyle Supports for Prader-Willi Syndrome
- Frequently Asked Questions About Prader-Willi Syndrome
- Prader-Willi Syndrome Resources Directory
Understanding Prader-Willi syndrome – Essential Resources and Information for Families, Health Professionals, and Caregivers
Prader-Willi syndrome is a rare condition that remains unfamiliar to many, including carers, parents, and family members. To help bridge this knowledge gap, we have curated a collection of research and resources dedicated to Prader-Willi syndrome. These valuable materials cater to families and individuals involved in the care and support of individuals living with Prader-Willi syndrome. Our aim is to provide accessible and up-to-date information and support to empower you.
Since 1979, Interaction has actively supported the Prader-Willi community, accumulating valuable insights and knowledge throughout the years. Whether you’re a carer or parent, this regularly updated guide is designed to help you navigate the complexities of Prader-Willi syndrome.
What is Prader-Willi Syndrome?
What Are the Symptoms of Prader-Willi Syndrome?
How Common is Prader-Willi Syndrome?
What Causes Prader-Willi Syndrome?
What Treatments are Available for Prader-Willi Syndrome?
The Future for People with Prader-Willi Syndrome
Accessing Supports for Prader-Willi Syndrome
Frequently Asked Questions About Prader-Willi Syndrome
Prader-Willi Syndrome Resources Directory
What is Prader-Willi Syndrome?
Summary:
- Prader-Willi syndrome is a rare genetic disorder that impacts development and growth, requiring special attention and care.
- People with Prader-Willi syndrome may experience an intense appetite, which, if not appropriately addressed, can lead to challenges with weight management and potential obesity.
- Individuals with this syndrome may exhibit short stature and intellectual disabilities, requiring further understanding and support.
- Access to comprehensive treatment and care provided by healthcare professionals can significantly enhance the overall quality of life for individuals with Prader-Willi syndrome. Prader-Willi syndrome (or PWS) is a rare and complex non-inherited genetic condition linked to the deletion or incompleteness of genes on the 15th chromosome. This chromosomal abnormality leads to neurological changes which cause altered growth patterns and development with associated cognitive disability and obsessive eating patterns (hyperphagia). While PWS presents unique challenges, modern advancements and methods have significantly improved the lives of individuals affected by the syndrome. These advancements enhance overall well-being and foster increased community engagement among individuals with PWS.
What are the Symptoms of Prader-Willi Syndrome?
Prader-Willi syndrome is a complex genetic disorder characterised by a range of signs and symptoms that can vary from person to person. These symptoms may also evolve and change gradually as individuals transition from childhood to adulthood.
Infants
When Prader-Willi syndrome (PWS) is recognised at birth, infants typically exhibit a variety of symptoms that indicate the presence of the condition. Common symptoms include:
1. Poor Muscle Tone (Hypotonia)
One of the primary signs observed in newborns with PWS is poor muscle tone, also known as hypotonia. Infants may display floppy movements and have a general lack of muscle strength. When held, they may feel limp or resemble rag dolls due to their decreased muscle tone.
2. Weakened Sucking Reflex and Poor Feeding
Babies with PWS often have a weakened sucking reflex, which can lead to difficulties in breastfeeding or bottle-feeding. The reduced muscle tone affects their ability to latch and effectively extract milk, resulting in poor feeding and inadequate weight gain. This can lead to failure to thrive if not addressed promptly.
3. Weak Cry and Poor Responsiveness
Infants with PWS may exhibit a weak cry and appear generally unresponsive to stimulation. They may seem unusually tired and have difficulty waking up. These signs can indicate the impact of the condition on their neurological development and overall energy levels.
4. Lack of Eye Coordination
Newborns with PWS may present with eye coordination issues, such as strabismus (abnormal eye alignment) or eyes turning towards one side. These eye coordination difficulties can potentially impact the visual development and perception of individuals with PWS.
5. Distinct Facial Features
Additionally, they may have distinct facial features, including almond-shaped eyes, a narrowing of the head towards the temples, and a narrow top lip with a turned-down mouth. These facial characteristics can aid in the early identification of PWS.
Recognising these symptoms at birth is crucial for timely diagnosis and appropriate management of Prader-Willi syndrome. Early intervention and comprehensive care can help address the associated challenges and improve long-term outcomes for individuals with PWS.
Early Childhood to Adulthood
As individuals with Prader-Willi syndrome grow into childhood and beyond, additional features may emerge and persist:
Food craving and weight gain: A hallmark symptom is a constant craving for food, leading to excessive eating, frequent snacking, and large portion sizes. This can result in rapid weight gain and ultimately obesity.
Underdeveloped sex organs (hypogonadism): Both males and females may experience underdeveloped sex organs, delayed or incomplete puberty, and infertility.
Poor growth and physical development: Insufficient production of growth hormones can lead to short stature, reduced muscle mass, and increased body fat. Other endocrine issues, such as hypothyroidism, may also be present.
Cognitive impairment: Mild to moderate intellectual disability is common, with individuals experiencing challenges in thinking, reasoning, and problem-solving. Learning disabilities may also be present.
Delayed motor development: Children with Prader-Willi syndrome may achieve physical milestones, such as sitting up or walking, later than their peers.
Speech problems: Speech development may be delayed, and individuals may struggle with articulation and speech clarity throughout their lives.
Behavioural problems: Some individuals may exhibit behavioural issues, including stubbornness, anger, control-seeking, and manipulative behaviours. Temper tantrums, especially when denied food, are not uncommon. Obsessive-compulsive behaviours and mental health disorders, like anxiety, may also arise.
Sleep disorders: Sleep disturbances, such as abnormal sleep patterns and sleep apnoea (pauses in breathing during sleep), can lead to excessive daytime sleepiness and exacerbate behavioural challenges.
Other signs and symptoms: Additional features may include small hands and feet, scoliosis (curvature of the spine), reduced saliva flow, vision problems, difficulty regulating body temperature, high pain tolerance, and hypopigmentation (pale hair, eyes, and skin).
It's important to note that while these are common signs and symptoms, the presentation and severity can vary widely among individuals with Prader-Willi syndrome. Regular monitoring, appropriate medical interventions, and comprehensive care can help manage the diverse challenges associated with this condition.
How is Prader-Willi Syndrome diagnosed?
There may be signs present in babies and early childhood that prompt health care providers to request blood testing for PWS. A definitive diagnosis is found via special genetic testing to identify abnormalities in chromosomes.
How does Prader-Willi Syndrome affect developmental milestones?
Babies and infants are often delayed in meeting developmental milestones such as sitting, crawling, walking, and talking.
Intellectual disability is present in varying degrees in most cases. Underdeveloped sex organs including undescended testes may be present in males, and both males and females may produce little or no sex hormones resulting in incomplete development at puberty and in most cases infertility.
Prader-Willi Syndrome and Behavioural Issues
Behavioural problems may develop in children with PWS. This includes psychological conditions, controlling and manipulative behaviour, as well as obsessive-compulsive and repetitive behaviours. Children and adults with PWS may have angry outbursts, particularly when denied food or when unable to handle changes to regular routine. Emotions and behaviour are often erratic and can be very challenging.
Prader-Willi Syndrome and Eating Habits
One of the most well-known symptoms of PWS is the preoccupation with food and constant craving and seeking of food. In the brain, the hypothalamus (part of the brain which controls hunger) is affected in people with PWS, leading to a strong psychological drive to eat as normal satiety (feeling of fullness) does not exist.
This drive to eat results in dangerous behaviours such as eating large quantities of food, food seeking behaviours (e.g., stealing, hoarding, eating from the garbage), and has potential for rapid weight gain and obesity if not carefully managed.
When to See a Doctor About Prader-Willi Syndrome
Regularly scheduled well-baby visits are highly important for recognising early signs of suboptimal growth and development, which may indicate the presence of Prader-Willi syndrome or other related conditions.
If you have any concerns about your baby's health or notice any concerning symptoms between these scheduled visits, it is crucial to promptly schedule an appointment with your child's doctor. This will allow you to openly discuss your observations and seek the necessary medical guidance without delay.
How Common is Prader-Willi Syndrome?
PWS is a rare and complex genetic condition, affecting roughly 400,000 people worldwide (or 1 in 10,000 - 30,000 worldwide).
In Australia, in 2010 at least 261 cases have been genetically confirmed and are seen in hospital based PWS clinics. One in 17,000 would be a conservative estimate of the birth incidence in the past two decades. Another 79, mainly older individuals with PWS are known to the PWS Association of Australia. Information on adults diagnosed with PWS is scarce and the total number of adult patients seen by specialists or general practitioners is currently unknown. Diagnosis of adults may be based on clinical characteristics only, which are not always confirmed genetically.
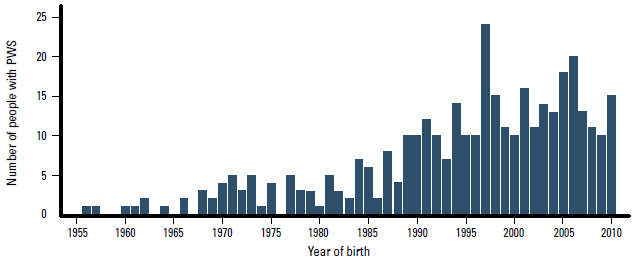
Number of people with Prader-Willi syndrome by year of birth in Australia since 1955.
Data from the Australian Prader-Willi syndrome database and the Prader-Willi Syndrome Association of Australia.
What Causes Prader-Willi Syndrome?
Summary:
- Prader-Willi syndrome (PWS) is a genetic disorder caused by inconsistencies in genes related to chromosome 15, which affect gene expression.
- PWS impacts the hypothalamus, causing uncontrollable hunger, lack of satiety, stunted growth, underdeveloped sex hormones, and disruptions in emotional expression, sleep cycles, and other bodily functions.
- Complications of PWS include obesity-related issues such as type 2 diabetes, high blood pressure, heart disease, sleep apnoea, and an elevated risk of liver disease and gallbladder stones.
- Insufficient hormone production in PWS leads to complications such as sterility and an increased risk of osteoporosis.
- Other complications can arise from binge eating, reduced quality of life, and the need for a collaborative care approach involving healthcare professionals, educators, therapists, and family members.
- Prader-Willi syndrome is a genetic disorder caused by inconsistencies of genes related to chromosomes 15. The exact mechanisms responsible for causing PWS are unknown, but the errors related to chromosome 15 impact the way genes are expressed, or how genes turn ‘on’ or ‘off’.
While the specific causes for the chromosomal errors remain unclear, research indicates that this happens for one of three reasons:
1. Paternal genes on chromosome 15 are missing
2. Errors or defects in paternal genes on Chromosome 15
3. Two copies of chromosome 15 from the mother are inherited by the child and no chromosome 15 from the father
How Prader-Willi Syndrome Impacts the Hypothalamus
The hypothalamus (the part of the brain which controls hunger and thirst and hormones related to growth and sexual development) functions differently in people with PWS. This disruption of a functioning hypothalamus results in:
- Uncontrollable hunger
- Lack of satiety
- Stunted growth
- Underdeveloped sex hormones
- Affected emotional expression, sleep cycles and other body functions
Complications of Prader-Willi Syndrome
Obesity-related complications
In addition to experiencing constant hunger, individuals with Prader-Willi syndrome often have low muscle mass, leading to a lower caloric requirement and reduced physical activity. This combination of factors increases their susceptibility to obesity and the associated medical issues, including:
- Type 2 diabetes
- High blood pressure, high cholesterol, and heart disease
- Sleep apnoea
- Other complications such as an elevated risk of liver disease and gallbladder stones
- Complications related to inadequate hormone production.
Insufficient hormone production complications
In Prader-Willi syndrome, there is a deficiency of various hormone levels. Hormones, which are released by the endocrine glands in the body, play a vital role in regulating numerous aspects of life, such as development, growth, puberty, reproduction, and metabolism.
Sterility: While there have been a few reported cases of women with Prader-Willi syndrome becoming pregnant, most individuals with this disorder are unable to conceive.
Osteoporosis: Low levels of sex hormones and possibly growth hormones in individuals with Prader-Willi syndrome place them at an increased risk of developing osteoporosis. This condition weakens bones, making them more susceptible to fractures.
Other complications
Additional complications that can arise from Prader-Willi syndrome include:
Effects of binge eating: Binge eating, characterised by consuming large quantities of food rapidly, can lead to abnormal enlargement of the stomach. People with Prader-Willi syndrome may not express pain, and vomiting is rare. Binge eating can also increase the risk of choking. In rare cases, excessive eating can even result in stomach rupture.
Reduced quality of life: Behavioural challenges associated with Prader-Willi syndrome can impact family dynamics, hinder educational progress, and limit social participation. These difficulties can significantly diminish the overall quality of life for children, teenagers, and adults with Prader-Willi syndrome.
Taking a collaborative care approach involving healthcare professionals, educators, therapists, and family members can ensure comprehensive support for individuals with Prader-Willi syndrome. Regular communication, coordinated care plans, and shared goals can heighten outcomes and promote an improved quality of life.
What Are the Symptoms of Prader-Willi Syndrome?
Summary:
Common symptoms of Prader-Willi syndrome are:
- Increased appetite;
- low muscle mass and tone;
- delayed growth and physical development;
- behavioural and mental health issues;
- and additional symptoms.
Prader-Willi syndrome presents with many symptoms that can affect a person’s physical, psychological, cognitive, and behavioural development. While some symptoms are more common than others, we have outlined the more general symptoms that affect people with PWS below.
Increased appetite and high propensity to obesity
One of the most well-known symptoms of PWS is the constant craving for food. People with PWS do not experience normal satiety (feeling of fullness) which, when unmanaged, often leads to overeating and obesity.
This symptom normally starts at around age two and can be accompanied by other behavioural issues related to eating such as hiding and hoarding food.
Low muscle mass and muscle tone
A key sign during infancy of PWS is poor muscle tone. This can appear in babies and infants as the ‘floppiness’ of limbs which is especially apparent when being held. The medical term for this symptom is hypotonia and can also present in the following ways:
- Poor reflexes, including suck reflexes when nursing
- Weak cry
- limited range of movement
Behavioural and mental health issues
It's important to note that individuals with Prader-Willi syndrome may experience various behavioural issues that can sometimes manifest as temper tantrums. Due to the complex nature of PWS and its impact on neurodevelopment, individuals with PWS may exhibit challenging behaviours that require a combination of treatments to manage. Other behavioural issues include:
- Strict adherence to routines;
- Obsessive compulsive or repetitive tendencies;
- Controlling or manipulative tendencies;
- Mental health issues such as depression and anxiety, often accompanied by skin picking
- Learning difficulties; and mild to moderate intellectual disability is common for people with PWS, which often means it is difficult for a child with PWS to reach developmental milestones. Problem solving and reasoning are commonly affected.
Other symptoms of Prader-Willi Syndrome
While the common symptoms of PWS have been outlined above, the following symptoms may also be present in someone who has PWS:
- Speech difficulties;
- Gastric complications like constipation, poor digestion and slow gastric emptying;
- Poor temperature sensation and regulation;
- High pain threshold – making it difficult to diagnose illness;
- High threshold for vomiting;
- slow sensory reception and processing;
- scoliosis or kyphosis;
- thick saliva and poor dentition;
- strabismus;
- sleep abnormalities including narcolepsy, excessive sleepiness and apnoea;
- hip dysplasia;
- short stature, small hands and feet;
- and lack of sexual maturity.
Navigating Prader-Willi Syndrome – Support is Available for You and Your Loved Ones
At Interaction, we understand the challenges that come with managing behavioural issues in individuals with PWS. Our team of experts is well-versed in developing personalised approaches to address these challenges. We can provide guidance, support, and practical strategies to help individuals with PWS and their families effectively manage and navigate through the PWS journey.
What Treatments are Available for Prader-Willi Syndrome?
- Early diagnosis and treatment are important for improving the health and well-being of people with Prader-Willi Syndrome (PWS).
- Treatment options for PWS depend on individual symptoms and challenges, and may involve the services of dietitians, physiotherapists, and psychologists.
- Some of the pathways to managing PWS includes: weight management strategies; mental health and behavioural treatments; sleep treatments; and growth and sex hormone therapy. While there is no cure for Prader-Willi syndrome, early diagnosis and treatment can improve the health and wellbeing of people with PWS. Medical and lifestyle supports are essential to addressing the symptoms of PWS and can include the services of allied health professionals such as dieticians, physiotherapists, and psychologists.
Common symptoms associated with PWS
PWS affects people differently. This is why there is no standard set of recommended treatments for people with PWS. Treatment options will depend on the specific challenges and symptoms present in each individual case, however interventions and treatments may address the following common symptoms of PWS:
- Excess weight and overeating
- Poor mental health
- Behavioural issues
- Sleep apnoea
- Delayed sexual development
Treatment options for people with PWS
Weight management
It is common for people with PWS to experience excess weight due to issues regulating hunger. Dietitians can assist in creating nutrient rich meal plans that restrict calorie intake to maintain a healthy weight. In addition, weight management options can also include daily exercise to offset the risk of obesity and other physical symptoms associated with PWS in including reduced muscle mass.
Mental health and behavioural treatments
Obsessive-compulsive tendencies, skin picking, and mood disorders are associated with PWS. Psychologists, counsellors, and psychiatrists can help with addressing poor mental health symptoms that are common with PWS.
Sleep treatments
Sleep apnoea and other sleep disorders are a common symptom of PWS. There are several treatments for sleep disorders, depending on the specific symptoms experienced, but common treatments involve lifestyle changes, surgery or the use of sleep apparatuses such as mouth guards.
Growth and sex hormone therapy
To assist with development and growth, an endocrinologist might administer hormone therapy. This may help with developing muscle mass, and primary and secondary sex characteristics. People with PWS are at higher risk of obesity and associated health concerns such as diabetes, high blood pressure, heart disease, sleep apnoea and joint/mobility issues. It is imperative from early on to set clear food guidelines and education around correct types and amounts of food that should be consumed, this includes being inventive with food items deemed as treats. Exercise plays an important role for people with PWS and introducing it as part of daily routines early on is recommended.
Care and attention to individual needs
By fostering a supportive and understanding environment and implementing appropriate behavioural interventions, we can work towards minimising the impact of these challenging behaviours and improving overall well-being for individuals with PWS.
The Future for People with Prader-Willi Syndrome
In the past, many people with Prader-Willi Syndrome (PWS) had a shorter than average life expectancy; with many passing in young adulthood due to health-related issues caused by the complexities of the condition. Although there is no cure for PWS, we now thankfully see great growth in the knowledge, research, medications, and intervention needs for people with PWS resulting in greater quality of life.
There is no question that people with PWS need lifelong support surrounding food and diet, however with the right supports, they can successfully lead lives much like their peers including finishing schooling, entering the workforce, and moving out into their own homes.
At Interaction, we are dedicated to providing the necessary resources, advocacy, and assistance to support individuals with PWS in reaching their goals and living their lives to the fullest. Together, we can make a positive difference in their journey towards independence and well-being.
Accessing Supports for Prader-Willi Syndrome in Sydney
While there have been significant strides in research, there's still so much more to discover about this complex condition. Considering it's a lifelong journey, continuous research, training, and education is fundamental.
Here at Interaction, we have an exceptional team of highly trained and experienced professionals who specialise in Prader-Willi Syndrome. We're here to offer a helping hand, support, and advice tailored specifically for individuals and families dealing with PWS. We understand that it's not an easy road, and we're dedicated to providing compassionate guidance to address your unique needs.
We firmly believe in empowering individuals with PWS and their families by offering the resources and assistance they require. Our goal is to be there for you every step of the way, ensuring you have the support and information needed to navigate this journey.
Support for Infants and Children with Prader-Willi Syndrome
Seek Valuable Specialist Care Where Possible
Children with Prader-Willi syndrome will benefit enormously from specialist care. Health professionals involved in their care often include:
General Practitioner (GP): A primary care doctor who provides overall medical care and coordinates specialised care for the child.
Paediatrician: A doctor specialising in the treatment and care of children, particularly in addressing the specific needs and challenges associated with Prader-Willi syndrome.
Dietitian: An expert in nutrition who can develop individualised meal plans, address the unique dietary requirements, and help manage weight-related concerns.
Physiotherapist: A healthcare professional who assists with physical therapy, exercises, and mobility, promoting motor development and strength.
Speech Therapist: A specialist who helps with speech and communication difficulties, providing strategies to improve language skills and oral motor function.
Dentist: A dental professional who focuses on oral health and addresses any specific dental concerns associated with Prader-Willi syndrome.
Optician: An eye care specialist who can assess and monitor visual health and provide appropriate corrective measures related to Prader-Willi Syndrome.
Behavioural Psychologist: An expert who helps address behavioural challenges and provides strategies for managing emotional and psychological well-being.
Genetic Counselling and Prader-Willi Syndrome
Seeking the guidance of a genetic counsellor can be valuable if your child has been diagnosed with Prader-Willi syndrome. Genetic counsellors are trained professionals who can provide emotional support and help you understand the condition, its causes, and the implications of the diagnosis for your child's health and development. They tailor their information and support to your family's circumstances, culture, and beliefs.
Support for Adults with Prader-Willi Syndrome
People with Prader-Willi syndrome have their own unique aspirations and dreams, just like everyone else. They greatly value and appreciate the support of those around them in pursuing their goals, while ensuring their safety and productivity. Interacting with individuals with PWS can be a truly joyful experience, as they often possess remarkable charisma, friendliness, and a deep sense of care and empathy. They are individuals who can bring warmth and positivity into your life, and their unique perspectives and personalities make them a delight to know and spend time with.
Maintain medical care and Intervention therapies
Due to the complexities of PWS, people with PWS are not able to accurately monitor their own health and wellbeing. Regular medical check-ups are essential in the maintenance of good health and wellbeing of adults with PWS. The person with PWS relies on those supporting them need to keep a watchful eye on changes in their health and behaviour that indicate a problem highlighted below:
- Individuals with PWS often have a high threshold for pain, which means they may not express discomfort until an injury or infection becomes severe.
- Fatigue and tiredness can serve as potential indicators of underlying illness in individuals with PWS.
- Increased bruising and swelling are frequently observed in individuals with PWS.
- People with PWS may experience a general sense of feeling unwell without being able to identify the specific source of pain.
- Vomiting is uncommon in individuals with PWS, and its occurrence may suggest a serious medical condition requiring immediate attention.
- Effective management of diabetes in individuals with PWS involves strict adherence to a low-calorie diet and a regular exercise regimen.
Regular and supported employment
Individuals with Prader-Willi syndrome have varying abilities and skills that can enable them to engage in different employment options. Depending on their capabilities, individuals with PWS can pursue opportunities in mainstream employment, disability supported employment, day program settings, or volunteer work.
Since 1979, Interaction has collaborated with prospective and current employers of individuals with PWS. Their goal is to create an inclusive and supportive work environment that allows employees with PWS to thrive and contribute as valuable members of the workforce.
Recreation and Community Engagement
Like all humans, adults with Prader-Willi syndrome find joy in actively participating in community life, engaging in conversations, and having a laugh. As you build a connection with them, you'll uncover their diverse range of interests and life experiences, which they will undoubtedly be delighted to share with you.
Incorporating regular physical exercise remains important as individuals with PWS transition into adulthood. Activities like strolling along the beach or taking the dog for a walk serve as valuable forms of incidental exercise. It is equally crucial for them to feel a sense of belonging and contribute to the broader community, in addition to pursuing educational or professional endeavours.
Accommodation and Housing
Deciding when a person with Prader-Willi syndrome (PWS) should move out of the family home is a personal choice that only the individual and their family can make. Once that decision is made, it’s important to explore available housing options that can meet the complex requirements of someone with PWS. Different stages of life may call for different housing solutions, and what works for one person may not work for another. Each family must carefully consider the needs and available support to make the best decision for their loved one with PWS.
Other Lifestyle Supports for Prader-Willi Syndrome
Interaction Disability Services is a compassionate not-for-profit organisation located in Sydney and the Central Coast and our primary objective is to provide support and empowerment in all aspects of life to individuals with Prader-Willi syndrome (PWS). Interaction works closely with you to build a support system that fits your individual needs and circumstances.
As an NDIS registered organisation, we are dedicated to connecting you with skilled support workers who have experience in assisting individuals with PWS. Additionally, we can assist in accessing a comprehensive range of services tailored to the needs of children, adults, and their families. Our commitment is to enhance the lives of those affected by PWS and ensure they receive the support they require.
Frequently Asked Questions About Prader-Willi Syndrome
What are the 5 primary signs of Prader-Willi syndrome?
The five primary signs of Prader-Willi syndrome (PWS) include poor muscle tone (hypotonia) during infancy, feeding difficulties and failure to thrive, characteristic facial features (almond-shaped eyes, narrowing of the head at the temples, thin upper lip), underdeveloped sex organs and delayed puberty, and a constant craving for food leading to excessive eating and rapid weight gain.
What is the life expectancy of a person with Prader-Willi syndrome?
The life expectancy of a person with Prader-Willi syndrome can vary depending on individual factors and the management of associated health conditions. However, with proper care, support, and early intervention, individuals with PWS are now living into adulthood and beyond, with the average life expectancy being around 60 years.
Is Prader-Willi syndrome a type of autism?
Prader-Willi syndrome is not a type of autism. While both conditions can have overlapping features and affect cognitive function and behaviour, they are distinct disorders. PWS is a genetic disorder caused by the loss of specific genes on chromosome 15, whereas autism spectrum disorder (ASD) is a neurodevelopmental disorder characterised by challenges in social interaction, communication, and repetitive behaviours.
What do people with Prader-Willi syndrome look like?
People with Prader-Willi syndrome often exhibit distinct facial features, such as almond-shaped eyes, a narrowing of the head at the temples, a thin upper lip, and a downturned mouth. However, it's important to note that the physical appearance of individuals with PWS can vary, and not all individuals will have all the characteristic features. Additionally, as they grow older, individuals with PWS may develop obesity due to the constant craving for food and a slower metabolism.
Why does my child have Prader-Willi syndrome?
Prader-Willi syndrome is relatively common among rare diseases, affecting 1 in 10,000 to 1 in 30,000 individuals. It is caused by a spontaneous genetic change during or near conception, usually involving missing paternally inherited genes on chromosome 15. In some cases, it can be inherited from an unaffected father. Remember, this is no one's fault, as genetic changes can occur naturally. Consulting a genetics doctor can provide more detailed information.
My child has Prader-Willi syndrome – what can I expect?
Remember to take a deep breath and be there for your child with Prader-Willi syndrome (PWS). Your support and presence are invaluable for their well-being and development. People with PWS lead fulfilling lives and can achieve great things with support. They can complete school, find employment, and gain independence. Family and community support are paramount for them to reach their highest potential and prevent obesity-related complications.
Optimising your child's care involves consulting various medical providers, including a geneticist, endocrinologist, nutritionist, pulmonologist, and therapists. Early intervention services are also important for their success. Growth hormone treatment should be initiated once the diagnosis is confirmed, as it helps with growth, maintaining lean body mass, and long-term cognition.
What will feeding be like?
Newborns with PWS often have difficulty feeding due to low muscle tone and disinterest in eating. After this phase, your child may feed normally for a period. However, individuals with PWS eventually struggle with achieving satiety, which may require environmental modifications to restrict access to food. While there is currently no treatment available, ongoing research is developing medications to address this issue.
What are the behavioural problems associated with PWS?
In early childhood, behaviours in children with PWS may resemble those of typical toddlers, including tantrums, routine dependence, transitioning difficulties, and stubbornness. They may also exhibit obsessive-compulsive behaviours and manipulative tendencies. Transitioning challenges persist, and they may display autistic-like, attention deficit, and hyperactive symptoms. Psychosis, depression, and skin picking can also be prevalent. Managing these behavioural symptoms requires routine, structure, and positive reinforcement. Psychotropic medications may also be beneficial.
Can Prader-Willi syndrome be cured?
Currently, there is no cure for PWS. However, with appropriate management and support, individuals with PWS can lead fulfilling lives and achieve their potential. Treatment focuses on addressing the symptoms and associated health conditions to improve quality of life.
What are the common medical complications associated with Prader-Willi syndrome?
PWS is associated with various medical complications. These can include obesity, type 2 diabetes, sleep apnoea, scoliosis, hormonal imbalances, behavioural and psychiatric disorders, cognitive challenges, and gastrointestinal issues. Regular medical check-ups and a multidisciplinary approach to care are important in monitoring and managing these complications.
Is there support available for people affected by Prader-Willi syndrome?
Absolutely. Thanks to many dedicated organisations and individuals, there is now a network of support for Prader-Willi syndrome Australia-wide.
Since 1979, Interaction has been actively devoted to understanding the importance of medical and lifestyle supports for individuals with PWS. We work closely with you to develop a personalised support system that caters to your specific needs and circumstances. Our range of Prader-Willi supports includes assistance with accommodation, support coordination, behaviour support, psychology, community access, and self-care.
Prader-Willi Syndrome Resources Directory
Interaction has provided best-practice supports to people with Prader-Willi syndrome since 1992. We take a great deal of pride in sharing our knowledge and connecting you with leading experts in PWS. The following resources will assist you in learning more about PWS and the different supports available. If you have any questions, please contact us.
Other informative websites and organisations include:
The Foundation for Prader-Willi Research
https://www.fpwr.org/about-prader-willi-syndrome
A not for profit organisation working to eliminate the challenges of PWS through research and therapeutic development.
Prader-Willi Research Foundation of Australia
An organisation dedicated to improving clinical outcomes and treatments for people living with PWS. International Prader-Willi Syndrome Organisation
An international foundation providing support to national PWS associations, people living with PWS, their families and support networks all around the world.
Raising Children – PWS
Practical advice for parents of children living with PWS.
Prader-Willi Syndrome Association – PWSA Australia
Up to date information and resources regarding Prader-Willi syndrome.
Prader-Willi Syndrome Association- PWSA Victoria
Prader-Willi syndrome resources specific to Victoria.

 1300 668 123
1300 668 123